A phase I study of different doses and frequencies of pegylated recombinant human granulocyte-colony stimulating factor (PEG rhG-CSF) in patients with standard-dose chemotherapy-induced neutropenia
Introduction
Recombinant human granulocyte colony-stimulating factor (rhG-CSF) has been widely used for prevention and treatment for neutropenia induced by chemotherapy (1-3). However, rhG-CSF needs daily subcutaneous injection, which brings a lot of inconvenience and costs for patients. Pegylated rhG-CSF (PEG rhG-CSF) is the form of rhG-CSF through conjugating polyethylene glycol (PEG) and rhG-CSF (4-6). It has an increased plasma half-life and a longer sustained duration, allowing a single administration. And report demonstrated that the single-dose PEG rhG-CSF didn’t show any inferior efficacy and it is safe to meet the standard of multi-dose rhG-CSF treatment (7). In addition, PEG rhG-CSF was approved by the U.S. Food and Drug Administration (FDA) in 2002, and has been widely accepted as standard therapy for prevention and treatment of severe neutropenia.
The recommended dose of PEG rhG-CSF for chemotherapy-induced neutropenia was single-dose 100 μg/kg or a fixed dose of 6 mg per chemotherapeutic cycle. Previous studies indicated that the efficacy and safety of the dosage of PEG rhG-CSF in one chemotherapy cycle at 6 mg was well compared with 11 daily injections of rhG-CSF at 5 μg/kg/d in treating neutropenia (8-12). In addition, single dose of 100 μg/kg PEG rhG-CSF also displayed the similar protection function compared with daily rhG-CSF injection in patients receiving myelo-suppressive chemotherapy regimens (11,13,14). However, most patients who received standard dose of chemotherapy seldom experience severe myelosuppression but need daily injections of rhG-CSF in routine clinical practice. Although a few studies revealed that 100 μg/kg PEG rhG-CSF was safe and effective for patients who received less-intense chemotherapy regimen (15-19), further exploration is still needed to investigate that whether 100 μg/kg or 6 mg PEG rhG-CSF is suitable for these patients.
The present study aimed to investigate the optimized dosage and frequency of prophylactic PEG rhG-CSF for patients receiving standard chemotherapy with lighter myelosuppression, and improve the safety and cost-effectiveness of PEG rhG-CSF.
Materials and methods
Patients
Eligible patients were those who had pathologically confirmed solid tumors and aged 18–70 years. Other eligibility requirements included: 1) chemotherapy and radiotherapy naive; 2) Karnofsky score ≥70; 3) absolute neutrophil count (ANC) ≥1.5×109/L; 4) platelet count ≥100×109/L; and 5) adequate hepatic [serum bilirubin ≤1.5 times the upper limit of normal (ULN), and serum transaminase ≤2.5 times ULN] cardiac, and renal (serum creatinine ≤2.0 mg/dL) functions. And the exclusion criteria were: 1) patients with bone marrow metastases, brain metastases, or active or uncontrolled infection; or 2) patients who were pregnant or breast-feeding.
This study is a registered trial approved by the China FDA (registration number: 2011L00842). The study protocol was approved by institutional review board of the National Cancer Center/Cancer Hospital, Chinese Academy of Medical Sciences and Peking Union Medical College. All subjects provided written informed consent prior to participation. The study was undertaken in full accordance with the guidelines for Harmonization/Good Clinical Practice, the Declaration of Helsinki. This study was registered at ClinicalTrials.gov as NCT02486354.
Study design
This was a single-center, open-label, and dose-escalation study to assess the safety, and pharmacokinetic and pharmacodynamic properties of prophylactic administration of PEG rhG-CSF in patients with solid tumors who received standard dose of chemotherapy.
Escalating dose (30, 60, 100 and 200 μg/kg) of PEG rhG-CSF and fixed dose of chemotherapy were given. Eligible patients received 3-cycle chemotherapy with identical dose as first-line treatment every 3 weeks. Chemotherapy regimens included PC [paclitaxel 175 mg/m2, carboplatin (area under curve, 5)], and EC (epirubicin 90 mg/m2, cyclophosphamide 600 mg/m2), which were administered intravenously on the first day of the cycle.
As showed in Figure 1, patients received no PEG rhG-CSF in the first cycle of chemotherapy, but patients who experienced grade 3 or higher neutropenia (ANC <1.0×109/L) would then enter the cycle 2 and cycle 3. Patients received a single subcutaneous injection of prophylactic PEG rhG-CSF on d 3 in cycle 2, and received half-dose subcutaneous injection of PEG rhG-CSF on d 3 and d 5 in cycle 3, respectively.
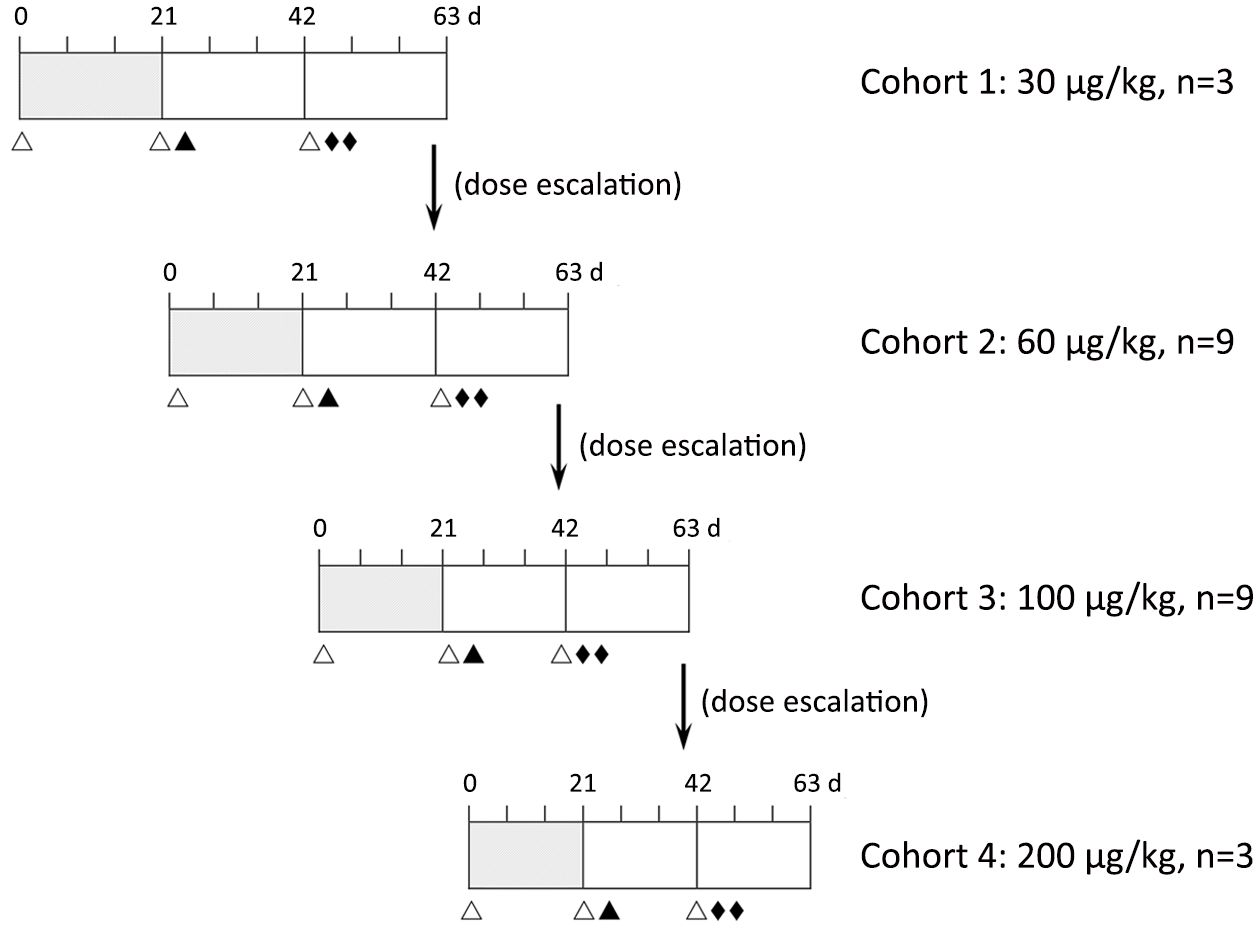
 , cycle 1 (blank control, and screening for patients with grade 3 or 4 neutropenia after chemotherapy);
, cycle 1 (blank control, and screening for patients with grade 3 or 4 neutropenia after chemotherapy);  , cycle 2 and cycle 3 [prophylactic pegylated recombinant human granulocyte-colony stimulating factor (PEG rhG-CSF) administration]; △, chemotherapy given at d 1 of each cycle; ▲, single dose of PEG rhG-CSF administrated at 48 h after chemotherapy in cycle 2;
, cycle 2 and cycle 3 [prophylactic pegylated recombinant human granulocyte-colony stimulating factor (PEG rhG-CSF) administration]; △, chemotherapy given at d 1 of each cycle; ▲, single dose of PEG rhG-CSF administrated at 48 h after chemotherapy in cycle 2;  , two half doses of the second cycle of PEG rhG-CSF administrated at 48 h and 96 h after chemotherapy in cycle 3.
, two half doses of the second cycle of PEG rhG-CSF administrated at 48 h and 96 h after chemotherapy in cycle 3.
Efficacy measurements
The primary efficacy endpoint was the incidence of grade 3 or 4 neutropenia after chemotherapy, and the duration of grade 3 or 4 neutropenia. The secondary endpoint was the incidence of febrile neutropenia (defined as ANC <0.5×109/L with auxiliary temperature >38.2 °C), and ANC profile.
Blood samples were obtained for complete blood counts (CBC) on d 1, d 3 to d 13, d 15, d 17, d 19, and d 21 of each cycle.
Pharmacokinetic measurements
In cycle 2, blood samples were collected at the following 17 time points for pharmacokinetic analysis: 0 h, 0.5 h, 2 h, 4 h, 8 h, 12 h, 16 h, 24 h, 36 h, 48 h, 72 h, 96 h, 144 h, 216 h, 288 h, 360 h and 432 h after subcutaneous injection of PEG rhG-CSF. In cycle 3, blood samples were collected at the following 18 time points: 0 h, 6 h, 12 h, 16 h, 24 h, 48 h (pre second dose), 54 h, 60 h, 64 h, 72 h, 84 h, 96 h, 120 h, 144 h, 216 h, 288 h, 360 h and 432 h after the first dose was administered. The blood samples were placed at room temperature for 30 min, and then centrifuged at 4,000 r/min for 10 min, and then the separated serum was stored at –80 °C until analysis. Samples were analyzed using enzyme-linked immunosorbent assay (ELISA).
Safety measurements
The safety was assessed in terms of adverse events and antibody formation. Vital signs and laboratory tests were also monitored. Serum was collected before PEG rhG-CSF administration, and at the end of cycle 2 and cycle 3, which were analyzed to detect the presence of immunoglobulin antibodies to PEG rhG-CSF by ELISA. Samples with values higher than established cut point were further confirmed by immunodepletion.
Study drug
PEG rhG-CSF was produced by HangZhou JiuYuan Gene Engineering Co., Ltd, China, and comprises protein rhG-CSF to which a 20-kDa PEG molecule is bound covalently to the N-terminal methionine residue. PEG rhG-CSF was supplied in single-use vials (0.6 mL containing PEG rhG-CSF 6 mg), and administered by subcutaneous injection.
Statistical analysis
Descriptive statistical analysis was performed in this study using SPSS software (Version 16.0; SPSS Inc., Chicago, IL, USA), P<0.05 was considered statistically significant. The mean, standard deviation, median, minimum and maximum were used to describe the measurement data, and frequency and percentage for the categorical data.
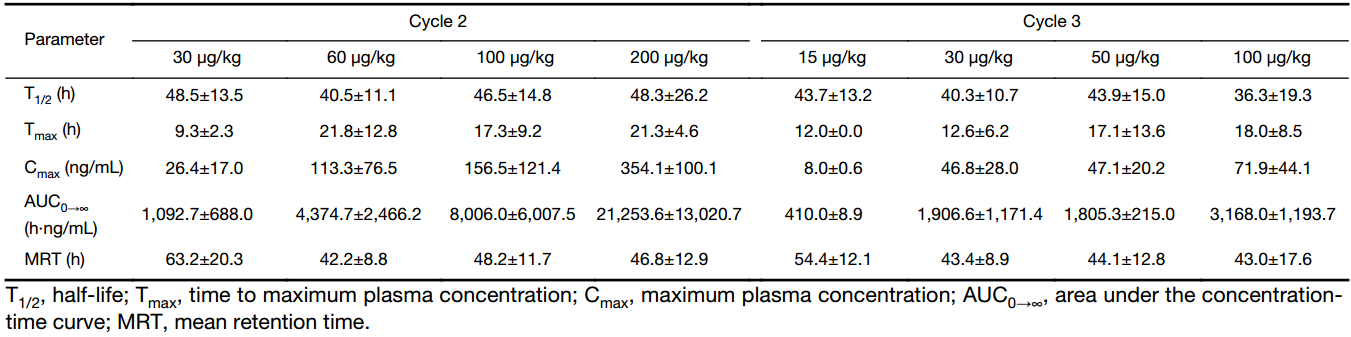
The pharmacokinetics and pharmacodynamic analysis of PEG rhG-CSF was performed using non-compartmental methods (WinNonlin 6.3, Pharsight Corporation, Mountain View, CA, USA) to obtain estimates of maximum plasma concentration (Cmax), time to maximum plasma concentration (Tmax), area under the concentration-time curve (AUC), and elimination half-life (T1/2). The pharmacokinetic parameters were compared between groups using one-way analysis of variance (ANOVA), and Kruskal-Wallis test was conducted when heterogeneity of variance occurred.
Non-compartmental methods were also used for analyzing ANC and CD34+ data, including the maximal ANC count (ANCmax), maximal CD34+ count (CD34+max), the time to the maximal ANC (TmaxANC) and CD34+ (TmaxCD34+), and the area under the effect-time curve (AUCANC and AUCCD34+). The relationship between serum concentrations and granulopoietic effects of PEG rhG-CSF was also evaluated.
Results
Patient characteristics
From February 16th, 2012 to January 28th, 2013, a total of 26 patients were enrolled into this study and received chemotherapy. Table 1 summarizes the baseline characteristics and patients’ distribution in different dose groups. Most patients were male (n=17) and had non-small cell lung cancer (n=21). Twenty-four patients received paclitaxel plus carboplatin, and two breast cancer patients received epirubicin plus cyclophasphomide.
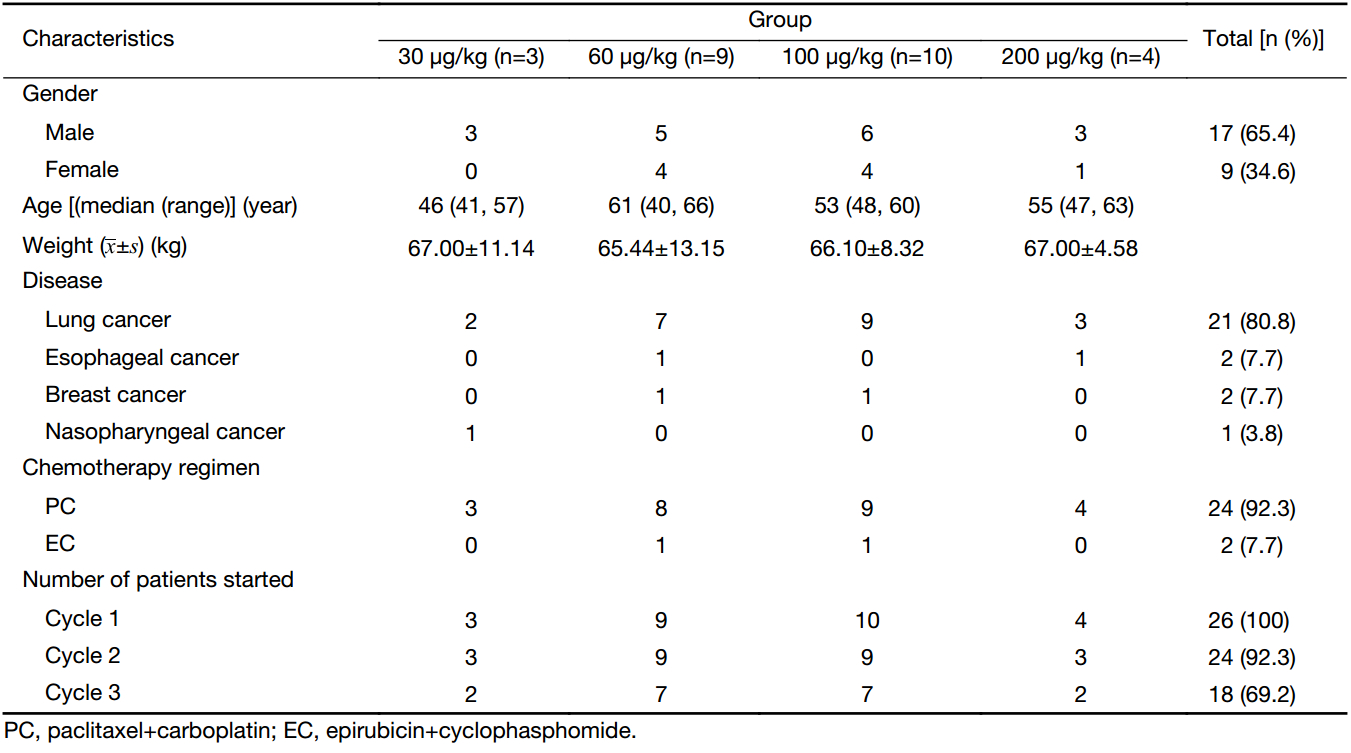
Full table
During cycle 1 and 2, patients withdrew due to not reaching grade 3 neutropenia or disease progression, and 24 patients entered and completed cycle 2 treatment. After 2-cycle treatments, 6 patients withdrew from the study due to disease progression, resulting in 18 patients entered cycle 3 treatment.
Neutrophil response
In cycle 1, chemotherapy induced grade 3 or 4 neutropenia in all patients (100%), in which 69.2% were grade 4 in severity. The median duration of grade 3 and grade 4 neutropenia were 5.5 (2.5–7.0) d and 2.5 (0.5–3.0) d, respectively. ANC began to decline around d 5 and d 6, reaching nadir on d 11 or 12, and then gradually recovered on d 17 to d 21. The mean ANC nadir was 0.30, 0.31, 0.61 and 0.31×109/L in single-dose PEG rhG-CSF of 30, 60, 100 and 200 μg/kg groups, respectively.
A lower incidence of grade 3 or 4 neutropenia was recorded in cycle 2 (7/24, 29.2%) and cycle 3 (0%) after PEG rhG-CSF treatment. In cycle 2, the incidence of grade 3 or higher neutropenia for patients receiving single-dose PEG rhG-CSF of 30, 60, 100 and 200 μg/kg was 66.67%, 33.33%, 22.22% and 0, respectively, with a median duration less than 1 (0–2) d. Grade 4 neutropenia was found in only two patients in 30 μg/kg dose group. No grade 3 or higher neutropenia was observed in cycle 3 in all dose cohorts.
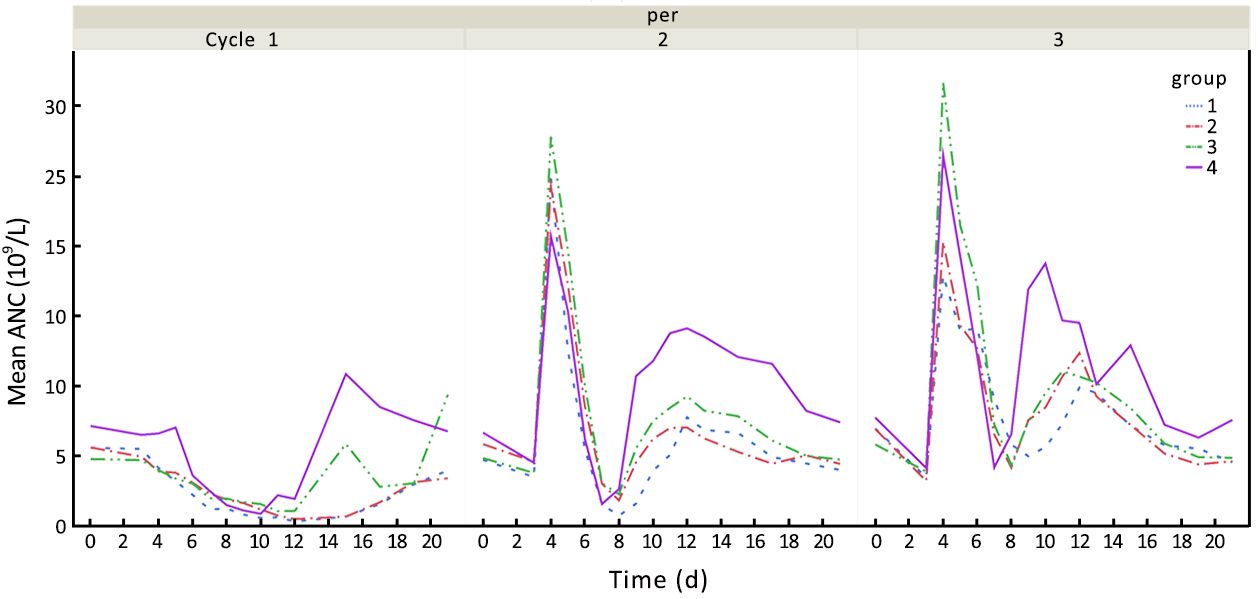
As showed in Figure 2, in cycle 2, the ANC peak was noted 1 d after a single-dose PEG rhG-CSF injection (d 4) in all dose cohorts, with a mean ANC of 24.86, 23.72, 27.81, and 20.21×109/L in 30, 60, 100 and 200 μg/kg dose group, respectively. The ANC peak was followed by the nadir around d 7 to d 8 with a mean ANC of 0.72, 1.73, 2.24, and 1.55×109/L, respectively. The ANC recovery was noted mostly on d 11 to d 13, with a mean ANC of 7.75, 7.04, 9.25, and 11.61×109/L, respectively. Double half-dose administration induced 2 ANC peaks in cycle 3 on d 4 to d 6, with a mean ANC of 17.88, 20.29, 31.66, and 26.5×109/L for 15, 30, 50 and 100 μg/kg cohorts, respectively. Double half-dose administration also produced a nadir on d 7 to d 8 with higher mean ANC, which was 2.89, 2.30, 2.36, and 2.51×109/L, respectively, for each dose cohort. Patients in the 200 μg/kg (double 100 μg/kg) exhibited an “overshoot” during the ANC recovery.
Six patients received rhG-CSF rescue (all in cycle 1), and 6 patients presented with febrile neutropenia (all in cycle 1). All patients with ANC recovered during the study observation period.
Pharmacokinetics
The mean serum concentration-time curves for PEG rhG-CSF are shown in Figure 3, and the pharmacokinetic parameters are summarized in Table 2. Both one single dose and double half-dose PEG rhG-CSF produced a sustained drug serum concentration. A non-linear pharmacokinetics profile of PEG rhG-CSF was exhibited over dose increasing in a dose and ANC-dependent manner. Significant difference in drug exposure was found between the two cycles. One single-dose administration in cycle 2 appeared to have higher Cmax and AUC values than those in cycle 3 in which double half-dose administration of PEG rhG-CSF was performed. There was no difference of T1/2, Tmax, and the mean retention time (MRT) between the two ways of PEG rhG-CSF administration.
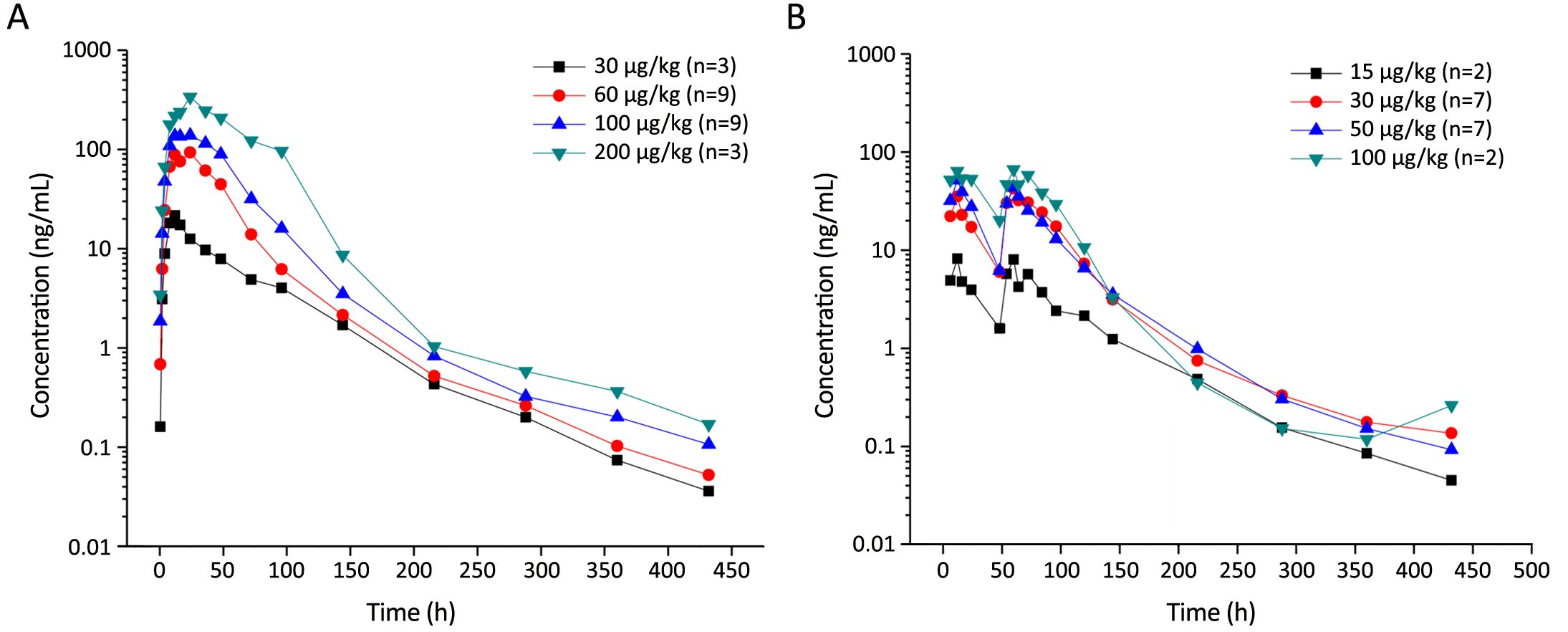
Safety
All patients reported at least one adverse event in this study, in which most were attributed to complications of chemotherapy. The most frequent PEG rhG-CSF-related adverse event was mild to moderate bone pain. The incidence, severity and duration of bone pain were similar between single-dose and double half-dose administration of PEG rhG-CSF. Escalating dose of PEG rhG-CSF was not observed to be associated with an increased incidence of bone pain. Anti-G-CSF antibody was detected in 7 out of 66 samples collected from the patients, in which 4 were detected in serum before PEG rhG-CSF administration. No evidence of neutralizing antibodies was found.
CD34+ cell mobilization
Significant inter-patient variability was detected on CD34+ cell mobilization, with a mean CD34+max ranged from 6.0 to 44.6 cells/μL over dose cohorts. There was no dose-effect relationship between dose and mean CD34+max. In cycle 2, the means of CD34+max were 21.0 cells/μL, 11.6 cells/μL, 6.0 cells/μL and 26.3 cells/μL for 30, 60, 100 and 200 μg/kg cohorts, respectively. In cycle 3, the means of CD34+max were 15.0 cells/μL, 12.7 cells/μL, 13.0 cells/μL and 44.6 cells/μL for double half-dose of 15, 30, 50 and 100 μg/kg cohorts, respectively. The median time to reach the maximal CD34+ cell counts was 10 d for both cycle 2 and 3, and the median time to recovery was 15 d for both cycles.
Discussion
The current study demonstrated that both single-dose and double half-dose PEG rhG-CSF are effective in the prevention of chemotherapy-induced neutropenia, and all dose cohorts showed favorable tolerability and pharmacokinetic profiles. Furthermore, no grade 3 or higher neutropenia was recorded when double half-dose prophylactic PEG rhG-CSF was given, suggesting double half-dose of administration may associated with better neutrophil response.
rhG-CSF is an effective prevention and management of chemotherapy-induced neutropenia and it can improve the patients’ quality of life (20-22). As its pegylated form, PEG rhG-CSF was reported to have a reduced clearance, increased plasma half-life, and sustained biologic activity, developing increased ANCs for substantially longer periods of time (23,24).
A series of studies have explored the efficacy of PEG rhG-CSF in patients receiving myelosuppressive chemotherapy. Johnston et al. demonstrated that a once-per-chemotherapy-cycle injection of PEG rhG-CSF at 100 μg/kg was as effective as daily injections of rhG-CSF at 5 μg/kg in reducing neutropenia (9). This finding was further confirmed by several randomized studies (10,25,26). One study compared single fixed-dose (6 mg) of PEG rhG-CSF with daily injection of rhG-CSF in breast cancer patients treated with doxorubicin and docetaxel, and found that PEG rhG-CSF provided similar neutrophil support to rhG-CSF in the treatment of febrile neutropenia, reducing the duration of grade 4 neutropenia and the depth of the neutrophil nadir (9). In another phase 3, double-blind study, 310 patients were randomized to receive 5 μg/kg daily injection of rhG-CSF or 100 μg/kg single-injection of PEG rhG-CSF (11). PEG rhG-CSF arm had a significantly lower incidence of febrile neutropenia than that in rhG-CSF arm (9% vs. 18%, P=0.029) (11). PEG rhG-CSF also revealed favorable efficacy and safety profile in patients receiving more-intense regimens. Vose et al. reported that PEG rhG-CSF was well compared with rhG-CSF in lymphoma patients treated with ESHAP chemotherapy (etoposide, methylprednisolone, cisplatin and cytarabine) (8), which is associated with high rates of neutropenic-related morbidity and occasional mortality (25,26). In addition, given the advantage of PEG rhG-CSF, including improved compliance and convenience, uninterrupted therapy, and simplifying the management of chemotherapy-induced neutropenia, it is also used in patients treated with standard dose of chemotherapy and less myelosuppressive. However, less-intense regimens may require fewer than 100 μg/kg of PEG rhG-CSF.
Our study indicated that both ways of PEG rhG-CSF administrations yield sufficient prophylactic neutrophil support, no patients was withdrawn from this study due to hematologic toxicity. In the blank control cycle 1, all patients reported to have reached grade 3 or higher neutropenia. The incidence of grade 3 or higher neutropenia was 66.7%, 33.3%, 22.2% and 0, respectively, after single dose injection of PEG rhG-CSF of 30 μg/kg, 60 μg/kg, 100 μg/kg and 200 μg/kg in cycle 2, which was well consistent with data from prior studies (9,16). Two half-dose administration of PEG rhG-CSF was found to have better outcome than one single dose administration in terms of reducing severe neutropenia, no patient endured grade 3 or higher neutropenia in any dose cohort after double half-dose injection in cycle 3. Moreover, two half-dose administrations were associated with an improved depth of the neutrophil nadir even at the lowest dose level, the mean ANC for the nadir ranged from 2.30 to 2.89 ×109/L in cycle 3 while 1.55 to 2.24×109/L in cycle 2, and 0.30 to 0.61×109/L in cycle 1. Reason for the better outcome from double half-dose of PEG rhG-CSF might be associated with the second ANC peak on d 6 induced by the second half-dose PEG rhG-CSF given on d 5, which makes up the ANC nadir on d 6 to 8 of the cycle. According to these findings, single dose of 60 μg/kg or 100 μg/kg, or double half-dose of 15 μg/kg or 30 μg/kg PEG rhG-CSF seem to be sufficient for the prevention of neutropenia induced by less-intense chemotherapy regimens.
Pharmacokinetic results of single dose PEG rhG-CSF in our study were consistent with those reported in prior studies (9,10,17,19), whereas the double half-dose administration failed to present increased AUC, MRT, and Cmax as expected. This contradiction between improved efficacy and decreased drug exposure may attribute to the neutrophil-mediated mechanism of PEG rhG-CSF clearance. PEG rhG-CSF is primarily eliminated by binding to the G-CSF receptor on the cell surface of neutrophils and neutrophil precursors (23). This characteristic makes PEG rhG-CSF rapidly cleared as neutrophil counts recover: a sharp increase of ANC in peripheral blood occurred shortly after the injection of PEG rhG-CSF, the large amount of ANC will consume the drug, resulting in a rapid decrease of PEG rhG-CSF in the serum. In cycle 3, double half-dose administration induced a higher increase than single dose PEG rhG-CSF in the second cycle, leading to an accelerated clearance of the drug, and a reduction of drug concentration in serum.
Conclusions
The pilot study demonstrated that double half-dose of PEG rhG-CSF had better efficacy compared with the single-dose administration in reducing incidence and duration of grade 3 or higher neutropenia. In addition, single dose of 60 μg/kg or 100 μg/kg, and double half-dose of 30 μg/kg PEG rhG-CSF per cycle produced similar neutrophil response in patients receiving less-intense chemotherapy regimens. However, the drug effectiveness in cycle 2 or the different patients participated in the 2 cycles (24 patients in cycle 2 and 18 patients in cycle 3) might cause the better therapeutic effect in cycle 3 than cycle 2. Therefore, further studies need to be carried out to investigate the therapeutic effect of double half-dose of PEG rhG-CSF next. Moreover, a dose-determining phase II study is currently ongoing (NCT01637493), which aims to compare single dose of 60 μg/kg, 100 μg/kg and double half-dose of 30 μg/kg administration of PEG rhG-CSF with rhG-CSF 5 μg/kg daily injection in patients who receive standard dose of chemotherapy.
Acknowledgements
The authors would like to thank all the investigators and patients who participated in this study. This work was supported by Hangzhou Jiuyuan Gene Engineering Co., Ltd, and partly funded by the Chinese National Science and Technology Major Project on Key New Drug Creation (2012ZX09303-012), and Beijing Municipal Science & Technology Commission Major Project for New Drug Innovation (Z111102071011001), China.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Welte K, Gabrilove J, Bronchud MH, et al. Filgrastim (r-metHuG-CSF): the first 10 years. Blood 1996;88:1907–29. [PubMed]
- Ozer H, Armitage JO, Bennett CL, et al. 2000 update of recommendations for the use of hematopoietic colony-stimulating factors: evidence-based, clinical practice guidelines. American Society of Clinical Oncology Growth Factors Expert Panel. J Clin Oncol 2000;18:3558–85. [PubMed] DOI:10.1200/JCO.2000.18.20.3558
- Lally J, Malik S, Whiskey E, et al. Clozapine-associated agranulocytosis treatment with granulocyte colony-stimulating factor/granulocyte-macrophage colony-stimulating factor: a systematic review. J Clin Psychopharmacol 2017;37:441–6. [PubMed] DOI:10.1097/JCP.0000000000000715
- Bond TC, Szabo E, Gabriel S, et al. Meta-analysis and indirect treatment comparison of lipegfilgrastim with pegfilgrastim and filgrastim for the reduction of chemotherapy-induced neutropenia-related events. J Oncol Pharm Pract 2017:1078155217714859.
- Kubo K, Miyazaki Y, Murayama T, et al. A randomized, double-blind trial of pegfilgrastim versus filgrastim for the management of neutropenia during CHASE(R) chemotherapy for malignant lymphoma. Br J Haematol 2016;174:563–70. [PubMed] DOI:10.1111/bjh.14088
- Brito M, Esteves S, André R, et al. Comparison of effectiveness of biosimilar filgrastim (NivestimTM), reference Amgen filgrastim and pegfilgrastim in febrile neutropenia primary prevention in breast cancer patients treated with neo(adjuvant) TAC: a non-interventional cohort study . Support Care Cancer 2016;24:597–603. [PubMed] DOI:10.1007/s00520-015-2818-2
- Delgado C, Francis GE, Fisher D. The uses and properties of PEG-linked proteins. Crit Rev Ther Drug Carrier Syst 1992;9:249–304. [PubMed]
- Vose JM, Crump M, Lazarus H, et al. Randomized, multicenter, open-label study of pegfilgrastim compared with daily filgrastim after chemotherapy for lymphoma. J Clin Oncol 2003;21:514–9. [PubMed] DOI:10.1200/JCO.2003.03.040
- Johnston E, Crawford J, Blackwell S, et al. Randomized, dose-escalation study of SD/01 compared with daily filgrastim in patients receiving chemotherapy. J Clin Oncol 2000;18:2522–8. [PubMed]
- Holmes FA, Jones SE, O’Shaughnessy J, et al. Comparable efficacy and safety profiles of once-per-cycle pegfilgrastim and daily injection filgrastim in chemotherapy-induced neutropenia: a multicenter dose-finding study in women with breast cancer. Ann Oncol 2002;13:903–9. [PubMed]
- Lyman GH, Reiner M, Morrow PK, et al. The effect of filgrastim or pegfilgrastim on survival outcomes of patients with cancer receiving myelosuppressive chemotherapy. Ann Oncol 2015;26:1452–8. [PubMed] DOI:10.1093/annonc/mdv174
- Kourlaba G, Dimopoulos MA, Pectasides D, et al. Comparison of filgrastim and pegfilgrastim to prevent neutropenia and maintain dose intensity of adjuvant chemotherapy in patients with breast cancer. Support Care Cancer 2015;23:2045–51. [PubMed] DOI:10.1007/s00520-014-2555-y
- Kam G, Yiu R, Loh Y, et al. Impact of pegylated filgrastim in comparison to filgrastim for patients with acute myeloid leukaemia (AML) on high-dose cytarabine (HIDAC) consolidation chemotherapy. Support Care Cancer 2015;23:643–9. [PubMed] DOI:10.1007/s00520-014-2417-7
- Cerchione C, Catalano L, Peluso I, et al. Managing neutropenia by pegfilgrastim in patients affected by relapsed/refractory multiple myeloma treated with bendamustine-bortezomib-dexamethasone. Support Care Cancer 2016;24:4835–7. [PubMed] DOI:10.1007/s00520-016-3430-9
- Grigg A, Solal-Celigny P, Hoskin P, et al. Open-label, randomized study of pegfilgrastim vs. daily filgrastim as an adjunct to chemotherapy in elderly patients with non-Hodgkin’s lymphoma. Leuk Lymphoma 2003;44:1503–8. [PubMed] DOI:10.1080/1042819031000103953
- Shi YK, Chen Q, Zhu YZ, et al. Pegylated filgrastim is comparable with filgrastim as support for commonly used chemotherapy regimens: a multicenter, randomized, crossover phase 3 study. Anticancer Drugs 2013;24:641–7. [PubMed] DOI:10.1097/CAD.0b013e3283610b5d
- Shi YK, Liu P, Yang S, et al. Phase I clinical trail of intravenous pegylated recombinant human granulocyte colony-stimulating factor. Ai Zheng (in Chinese) 2006;25:495–500. [PubMed]
- Shi YK, He XH, Yang S, et al. Treatment of chemotherapy-induced neutropenia pegylated recombinant human granulocyte colony-stimulating factor: a multi-center randomized controlled phase II clinical study. Zhonghua Yi Xue Za Zhi (in Chinese) 2006;86:3414–9. [PubMed]
- Yamamoto N, Sekine I, Nakagawa K, et al. A pharmacokinetic and dose escalation study of pegfilgrastim (KRN125) in lung cancer patients with chemotherapy-induced neutropenia. Jpn J Clin Oncol 2009;39:425–30. [PubMed] DOI:10.1093/jjco/hyp038
- Anguita-Compagnon AT, Dibarrart MT, Paredes L, et al. Peripheral blood stem cell mobilization with a single dose of PEG-filgrastim in patients with multiple myeloma previously treated with radiotherapy. Leuk Lymphoma 2017:2724–7. [PubMed] DOI:10.1080/10428194.2017.1300895
- Aapro M, Bokemeyer C, Ludwig H, et al. Chemotherapy-induced (febrile) neutropenia prophylaxis with biosimilar filgrastim in elderly versus non-elderly cancer patients: Patterns, outcomes, and determinants (MONITOR-GCSF study). J Geriatr Oncol 2017;8:86–95. [PubMed] DOI:10.1016/j.jgo.2016.09.006
- Maul JT, Stenner-Liewen F, Seifert B, et al. Efficacious and save use of biosimilar filgrastim for hematopoietic progenitor cell chemo-mobilization with vinorelbine in multiple myeloma patients. J Clin Apher 2017;32:21–6. [PubMed] DOI:10.1002/jca.21459
- Yang BB, Kido A. Pharmacokinetics and pharmacodynamics of pegfilgrastim. Clin Pharmacokinet 2011;50:295–306. [PubMed] DOI:10.2165/11586040-000000000-00000
- Yang BB, Kido A, Salfi M, et al. Pharmacokinetics and pharmacodynamics of pegfilgrastim in subjects with various degrees of renal function. J Clin Pharmacol 2008;48:1025–31. [PubMed] DOI:10.1177/0091270008320318
- Holmes FA, O’Shaughnessy JA, Vukelja S, et al. Blinded, randomized, multicenter study to evaluate single administration pegfilgrastim once per cycle versus daily filgrastim as an adjunct to chemotherapy in patients with high-risk stage II or stage III/IV breast cancer. J Clin Oncol 2002;20:727–31. [PubMed] DOI:10.1200/JCO.2002.20.3.727
- Green MD, Koelbl H, Baselga J, et al. A randomized double-blind multicenter phase III study of fixed-dose single-administration pegfilgrastim versus daily filgrastim in patients receiving myelosuppressive chemotherapy. Ann Oncol 2003;14:29–35. [PubMed]